UMG and SubRed Therapeutics aim to jointly develop a therapy for treatment of a rare, devastating childhood disease
Göttingen, 14.6.2023
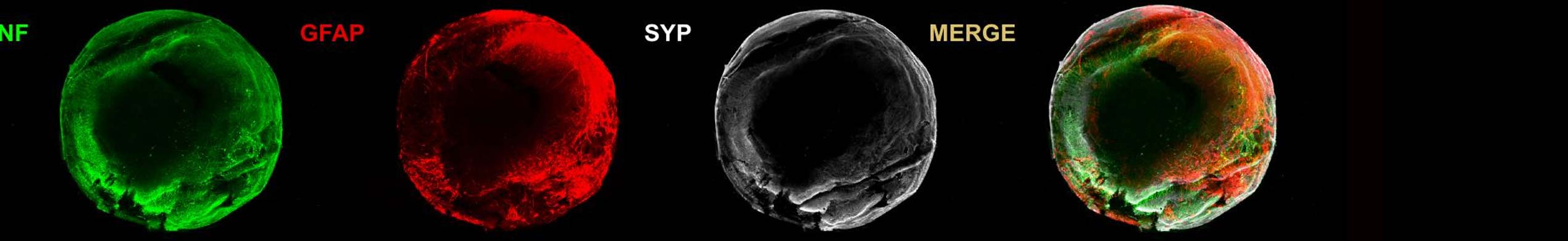
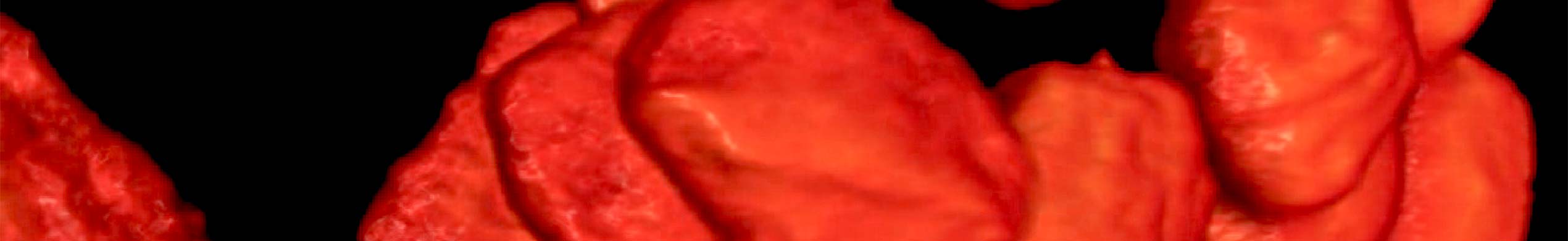
In the Department of Pediatrics and Adolescent Medicine at UMG, scientists led by Dr. Lars Schlotawa have developed a therapeutic approach that may lead to the first effective treatment of the rare neurometabolic disease MSD (multiple sulfatase deficiency). Through the mediation of MBM ScienceBridge, the Australian pharmaceutical company SubRed Therapeutics, a subsidiary of Tarnagulla Ventures, was chosen as a partner for further development of the therapeutic approach. The common goal of UMG and SubRed is to jointly develop a therapy and achieve its approval as the first drug for the treatment of MSD.
read more